Image by Marjon Besteman from Pixabay. Do I really need a knee replacement on a knee I’ve never had pain in, even though the X-ray shows arthritis?
You’ve had pain in your knee for a few years now and it has unfortunately gotten to the point where it is difficult to do the normal activities in your life. You go to the hospital and get an X-ray that shows you have osteoarthritis in not only your painful knee, but also your other knee that hasn’t bothered you at all! The surgeon wants to replace both knees, but you wonder to yourself; is this really necessary?
In this blog, I will discuss if it is possible to have knee arthritis without pain and if knee arthritis alone means you should get a knee replacement.
What is knee osteoarthritis?
Osteoarthritis is one of the leading causes of pain and disability.[1] Not only does osteoarthritis break down the cartilage of the knee, but it also damages the bones, muscles, ligaments, and fluid in and around the joint.[1] The knee is the most common joint to have osteoarthritis and is an important joint for bearing weight and doing everyday activities.[2] Knee osteoarthritis can make it difficult to walk, use the stairs and stand for any length of time.[3] To learn more about exactly what knee osteoarthritis is, read this blog.
Is it possible to have osteoarthritis in your knee and not feel it?
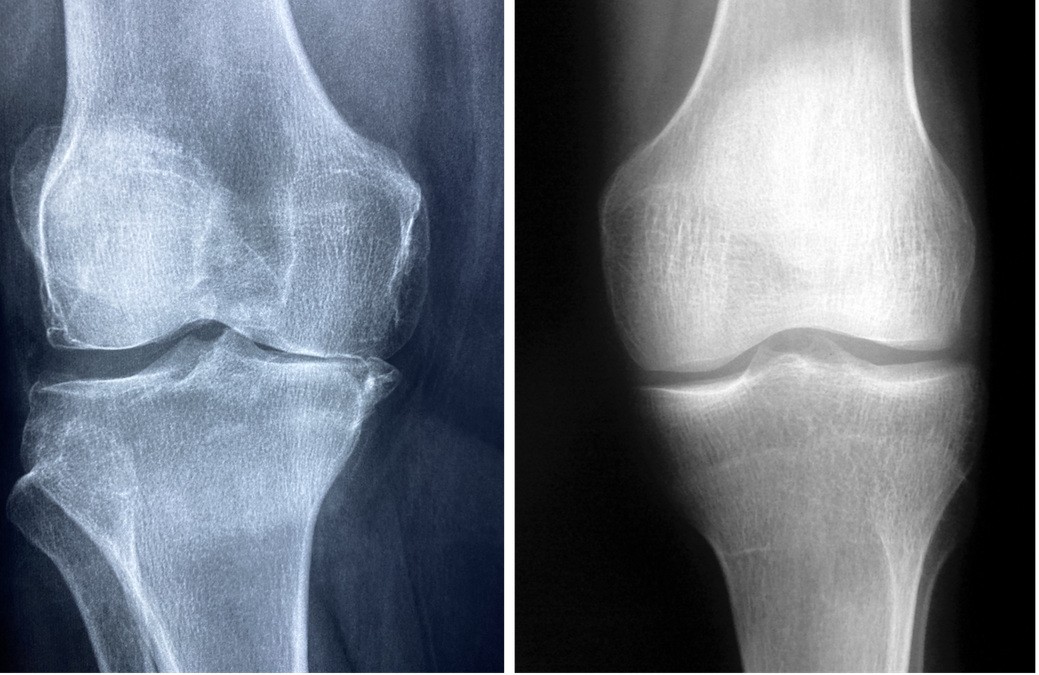
In healthcare, a common way of diagnosing osteoarthritis is through an X-ray. On an X-ray, knee osteoarthritis will show up as decreased joint space.[4] This is what people commonly refer to as ‘bone on bone’. With all of the damage that osteoarthritis does to the knee, and the effect this has on a person’s ability to do daily activities, it may be confusing to be told you have knee osteoarthritis after getting an X-ray, but you have no pain.
X-rays are an important tool in healthcare. Generally, the more severe that arthritis appears on an X-ray, the more likely it is that symptoms, such as pain, are present.[5] Although this is not always the case! While it is normal to have pain accompanied by an X-ray that shows knee osteoarthritis, it is actually just as common to have no pain. 44-53% of people with these positive X-ray findings have no pain in the knee.[5] This doesn’t mean that you should not have pain with arthritic X-ray findings, but rather it shows that X-ray findings ALONE are not a good tool to show if someone has knee pain or difficulty functioning, due to knee osteoarthritis.
The reason one person with an arthritic X-ray might have pain and another person might not is related to the person's leg strength, presence of other medical conditions, and mental health status.[3] Increased leg strength, proper management of other medical conditions, and good mental health are likely factors that contribute to having less pain in your arthritic knee.
Is it really necessary to replace a knee that has no pain?
If you have no pain in your knee, it is NOT necessary to have a knee replacement; even if your doctor wants you to get one. You and your doctor are a team. You work together. It is okay to disagree and it is important to voice your concerns because in the end, it is your knee. Even if you have an X-ray that shows knee arthritis, it does not mean you absolutely need a knee replacement. An X-ray showing arthritis is just one of three main factors used to consider if a knee replacement is necessary. The other two factors to consider before getting a knee replacement are if you have pain and how limited your daily activities are.[4]
In someone with knee osteoarthritis, the purpose of a knee replacement is to reduce pain and make it easier to do everyday activities. Even if you do have knee pain, before considering a knee replacement it is important to first try to manage your pain through physiotherapy.[4] But, if you have no pain and you can function with everyday activities, there’s nothing in your life that a knee replacement will improve. Therefore, if you have no pain and you can function throughout the day, you should not get a knee replacement.
If I have arthritis and no pain, what should I do? Can I avoid getting my knee replaced?
There are several things that can be done to prevent the progression of pain in people with osteoarthritis. The most important thing to do is move your knee. Physical activity and exercise helps in both the prevention and management of pain, and the ability to function with everyday activities, in people with osteoarthritis.[2] When determining the type of physical activity, it is most important to do what you enjoy, as this increases the likelihood of incorporating it into your lifestyle. It is also recommended to include a combination of aerobic exercises like walking or cycling, resistance exercises specifically targeting the knee muscles, and functional exercises to help you continue doing the things you love.[2]

A second thing to consider to prevent progression of pain in osteoarthritis is weight loss. If you are overweight there is more load on the joint, which can cause pain and reduce function.[6] Additionally, having excess fat tissue can further progress the destruction of the knee joint, further reinforcing the importance of weight loss.[6]
Lastly, living with osteoarthritis can take a toll on your mental health and it is important to recognize how mental health plays a big role in pain. The two interact in a terrible cycle. Poor mental health will cause increasing levels of pain, while pain also leads to poor mental health.[7] Keeping a positive attitude, staying physically active, and talking about your mental health can help reduce depression, which will reduce the risk of pain getting worse.[3] For more information on how to improve mental health due to injury or disease, read this blog. The National Institute of Mental Health is also a great resource to learn more or to find help.
Conclusion
You do NOT need a knee replacement in a knee you’ve never had pain in, even if an X-ray shows you have osteoarthritis. In addition to arthritic X-ray findings, knee pain and a decreased ability to do everyday activities need to be present to consider getting a knee replacement. To delay or decrease the likelihood of needing a knee replacement, there are several actions you can take. Most importantly, you should continue to move your knee by staying active with activities you enjoy. Additionally, if you are overweight, losing weight will help you decrease pain and improve physical function. Lastly, it is important to recognize the impact that good mental health has on pain prevention. Following these strategies will help keep your knee pain-free and prevent the need for a knee replacement. If you need further customized assistance during your surgery or injury recovery check out our Online Physical Therapy page to book your 1-on-1 video session with a physical therapist.
Whether you’re managing osteoarthritis or just had a knee replacement, the Curovate mobile physical therapy app is a great tool to use to help you decrease pain and get back to the activities you love. The app includes a personalized exercise program, video guided exercises, and the ability to track your progress, all from your phone! You can download the Curovate app from the App Store or the Play Store using the links below.
 |
 |
|---|
Other Blogs Related to Osteoarthritis and Knee Replacement
- What is Osteoarthritis?
- What is a Total Knee Replacement?
- Should I put off my total knee replacement surgery? What are my other options?
- The Mental Side of Injury: Hot to Keep a Positive Attitude During Recovery
- Is it normal to still have pain after a knee replacement surgery?
- Why does my knee feel weird after my total knee replacement? Why does my knee feel heavy after my total knee replacement?
References







