What is Patellofemoral Pain Syndrome (PFPS)? Patellofemoral pain syndrome (PFPS) is a condition where you may experience pain[1] in front of the knee, and around the kneecap and cracking and popping sounds behind the kneecap when keeping the knee bent for long periods of time, or climbing stairs.[2], [3], [5], [7], [8]
Why do I get pain around my kneecap? The patella is the bone that sits on top of your knee joint. Behind the patella, there is a layer of cartilage that allows it to smoothly glide over the groove of the femur (the thigh bone). There are fluid-filled sacs (bursae) and synovial fluid inside the knee joint that provide lubrication and allow for smoother gliding of the patella when the knee moves. The patella is also attached to collateral ligaments, muscles and skin. Collateral ligaments are bands of tissue that connect on the outer and inner side of the knee that connect the upper and lower leg.
PFPS can result from tightness in the Vastus Lateralis muscle, the muscle that pulls the patella up and outwards, and weakness in the Vastus Medialis Obliques muscle, the muscle that pulls the patella slightly in. Additionally, tightness in structures on the outside of the knee (Vastus Lateralis, Lateral Retinaculum and Iliotibial Band) can all pull the patella towards the outside. The Lateral Retinaculum is a band of tissues that lie on the outside portion of the patella, and helps keep the patella in the appropriate position. The Iliotibial Band is a thick band of tissues that runs on the outside portion of the hip and thigh, and attaches to the outside portion of the knee. It also helps promote appropriate positioning of the patella at the knee joint. Due to this, the back of the patella rubs on the surface of the femur. Continuous irregular pressure of the patella on the femur can lead to pain around the knee joint.[4],[14]
Who is most affected by the condition?Athletes who’s sport demands a lot of running, jumping, walking or cycling[6], and more women than men.[2]
What causes the condition?
Overuse syndrome and inactivity. When we increase our level of activity too fast and too soon, this can overload the joint and place a lot of stress between the kneecap and the femur, and can lead to pain. A sudden change in your activity levels such as jogging, running, jumping or climbing stairs. To avoid this, you should gradually increase your activity levels regardless of your new activity chosen.[1],[12] When keeping the knee bent for too long and remaining inactive, it will increase pain in the knee as well.[10] As with many types of knee pain, PFPS results from too much or too little activity.
Anatomical irregularity
Increased Q-angle - the Q-angle is a line that runs between the front pelvic bone to the middle of the patella. A typical angle in men is 12 degrees, and women is 17 degrees.[13] When the Q-angle is greater, there is maltracking of the patella where it moves slightly towards the outside of the knee. This causes the back of the patella to rub on the front surface of the femur, which causes pain.[13]
Muscular imbalances - Tight (or shortened) muscles around the knee joint → When there is tightness in the front-thigh muscle (Rectus Femoris), bending the knee (during sitting, running, squatting, or stair climbing) will cause increased pressure on the knee joint. Secondly, when the muscle on the outside of the knee (Iliotibial Band) is tight, it will attempt to pull the kneecap towards the outside of your knee, which leads to maltracking and eventually, pain.[9]
Weak muscles → Weakness of the inner thigh muscle can lead to the kneecap being pulled towards the outside of the knee, which can also lead to malalignment and pain.[11]
What would my symptoms be? The most common symptom is pain around the knee joint. More specifically, pain will increase with knee bending (squatting, prolong sitting with knees bent, or climbing stairs). There may also be cracking/popping sounds with knee movements.[3]
Treatment options
Activity modifications - If there is pain with activity, you want to change the intensity and duration of your activities. Start slow and then gradually increase the frequency of your training.[9] To learn more about active recovery check out this blog here!
If there is increased pain in the knee, use RICE. [12]
Rest - reduce the overall amount or intensity of activity especially if you have started a new activity such as jogging. Complete rest is not recommended for PFPS.
Ice - you can use an ice-compress OR an ice pack wrapped around the knee with a towel for 20 minutes.
Compress - you can wrap an elastic bandage around the knee.
Elevate - when resting, elevate the knee above the level of your heart. You can place your legs on an elevated surface when lying in bed.
Physical Therapy - your physical therapist will work on various treatments ranging from activity modifications, stretching tight structures and strengthening weak muscles
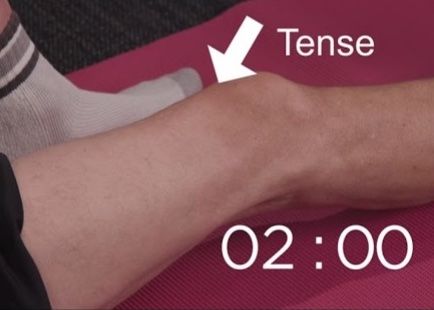
- Isometric - exercises where you are contracting the muscle without actually moving your knee.
- Quadriceps strengthening exercises - the quads are the muscles at the front of your thigh. An example of this is the first picture below.
- Straight leg raise - this is a simple exercise where you contract your quads and lift your leg up as you see in the second picture below.
Closed kinetic chain exercises - where the foot stays in contact with the ground while you do the exercise. These exercises place less stress on the knee joint. Some exercises include squatting or sitting to stand from a chair or bed.
VMO training - the vastus medialis Obliques (VMO) is a thigh muscle that sits on the inside of the knee joint. When this muscle is weak, it allows the patella to glide towards the outside of the knee joint - which can contribute to PFPS.
Having strong hip muscles will play a key role in preventing the patella from moving towards the outside of the knee joint during functional activities; thus, placing less stress on the knee joint and reducing the pain associated with patellofemoral pain syndrome.
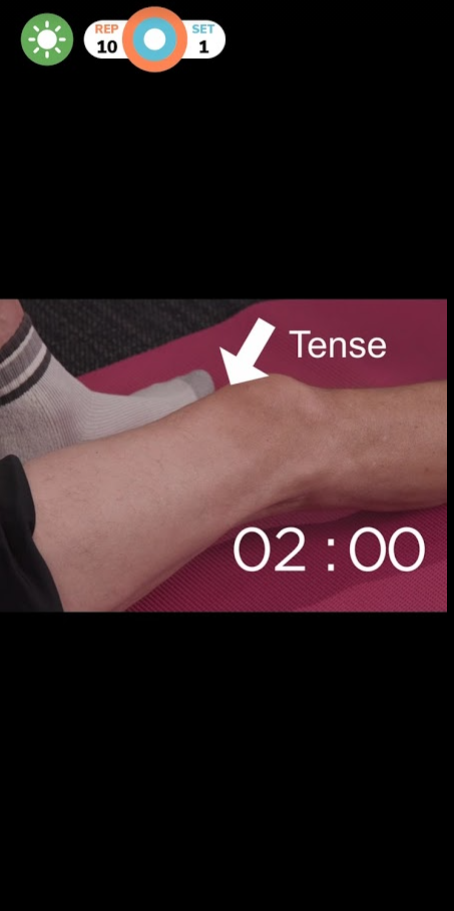

The images you see above are all from Curovate. Curovate is a rehabilitation app designed for knee replacement, hip replacement and ACL injury. With step by step videos, progress tracking and the ability to measure your range of motion, Curovate lets you start your recovery at home to get back to the things you love!
If you need further customized assistance during your surgery or injury recovery check out our Virtual Physical Therapy page to book your 1-on-1 video session with a physical therapist.
References
3. Cleveland Clinic. 2021. Patellofemoral Pain Syndrome.
4. Gudeman. 2000. OrthoIndy. Patellofemoral Syndrome (PFS).
5. Healthline. 2021. Patellofemoral Pain Syndrome.
6. Johns Hopkins. 2021. Patellofemoral Pain Syndrome.
7. Mayo Clinic. 2021. Patellofemoral Pain Syndrome.
8. Medical News Today. (2018). What’s to know about crepitus of the knee?
9. OrthoInfo. 2021. Patellofemoral Pain Syndrome.
10. OrthoCarolina. 2021. Patellofemoral Pain Syndrome (Runner’s Knee): What to know.
12. Physiopedia. 2021. Q-Angle.